Iron deficiency anaemia is a well‑recognised long‑term complication after bariatric surgery. Because these procedures alter the stomach and small intestine, they also change how nutrients—especially iron—are absorbed. Without proactive monitoring and supplementation, patients can develop iron deficiency or iron‑deficiency anaemia, sometimes severe enough to require intravenous treatment.
This guide explains why iron deficiency happens, how to recognise it, what BOMSS recommends, and how patients and clinicians can manage it effectively.
Why Bariatric Surgery Causes Iron Deficiency
Different bariatric procedures affect iron absorption in different ways, but several mechanisms are common:
1. Reduced Stomach Acid
Stomach acid helps convert dietary iron into a form the body can absorb. After sleeve gastrectomy or gastric bypass, acid levels drop significantly.
2. Bypassed Absorption Sites
Procedures like Roux‑en‑Y gastric bypass (RYGB) and one‑anastomosis gastric bypass (OAGB) bypass the duodenum and proximal jejunum, the primary sites of iron absorption.
3. Lower Dietary Intake
Many patients struggle with:
- Reduced appetite
- Intolerance to red meat
- Smaller portion sizes
These factors reduce iron intake long‑term.
4. Increased Requirements
Menstruating women are at particularly high risk due to ongoing blood loss.
How Common Is Iron Deficiency?
Studies consistently show high rates of deficiency:
- Up to 50% of patients after gastric bypass
- 10–30% after sleeve gastrectomy
- Higher risk 3+ years after surgery
- Many eventually require IV iron
BOMSS highlights that low ferritin is an early indicator, but normal or high ferritin does not rule out deficiency, especially if inflammation is present.
BOMSS‑Recommended Blood Monitoring
According to the BOMSS GP guidance (2023), iron status must be checked annually for life.
Annual tests include:
- Ferritin
- Full iron profile (especially if ferritin is high or inflammation suspected)
- Full blood count (FBC)
- Vitamin B12 & Folate (deficiencies often coexist)
BOMSS notes that ferritin alone can be misleading—full iron studies are more useful when ferritin is elevated due to inflammation.
Lifelong Iron Supplementation (BOMSS Guidance)
BOMSS recommends routine iron supplementation for all patients who have had:
- Sleeve gastrectomy (SG)
- Roux‑en‑Y gastric bypass (RYGB)
- OAGB with BP limb ≤150 cm
Standard doses (from BOMSS Table 2):
- Ferrous sulphate 200 mg once daily, OR
- Ferrous fumarate 210 mg once daily, OR
- Ferrous gluconate 300 mg twice daily
Higher doses for menstruating women:
- Twice daily dosing of the above preparations
Important BOMSS absorption advice:
- Take iron with food
- Avoid tea/coffee for 90 minutes around dosing
- Take iron and calcium at least 2 hours apart
When oral iron fails
Some patients—especially those with constipation, haemorrhoids, or poor absorption—may require parenteral (IV) iron.
Symptoms of Iron Deficiency After Bariatric Surgery
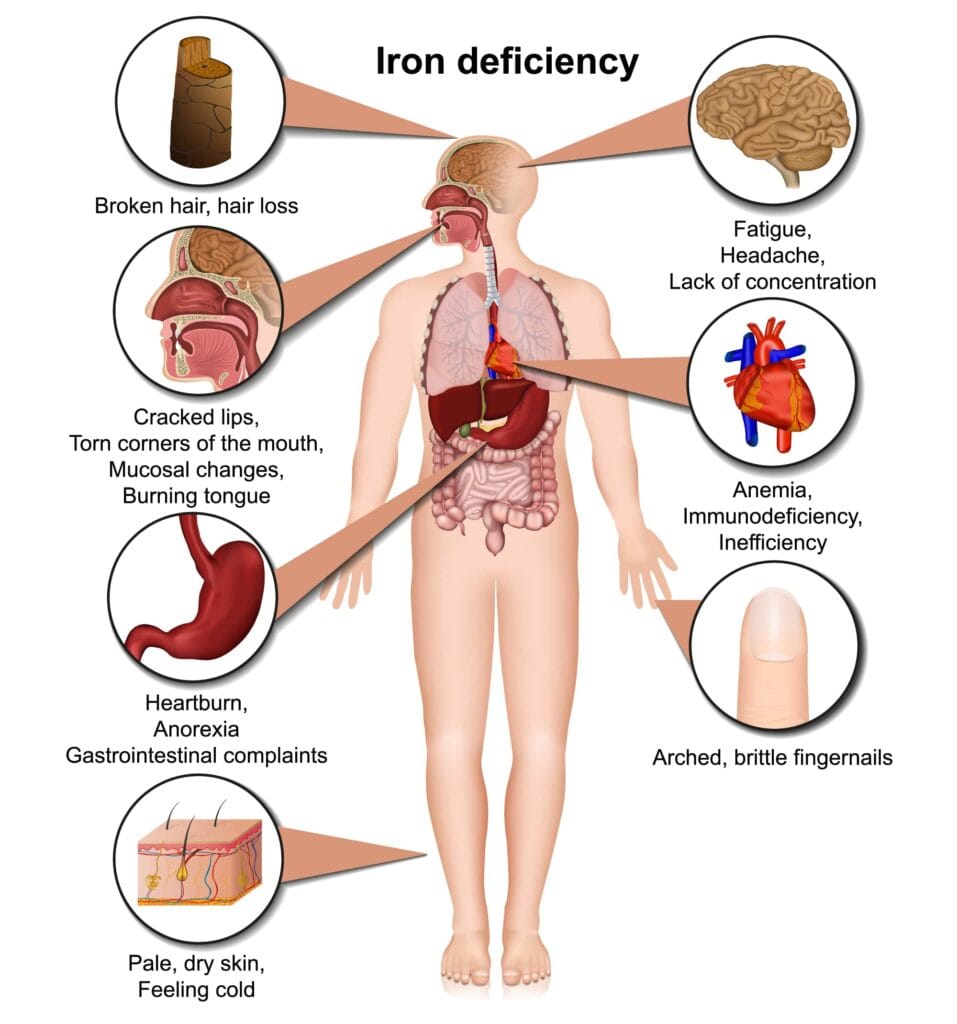
BOMSS lists iron deficiency as a cause of several symptoms:
Common signs:
- Fatigue, weakness
- Shortness of breath
- Pale skin
- Hair loss
- Glossitis (inflamed tongue)
- Poor wound healing
- Memory issues
Important BOMSS note:
If one deficiency is found, others are often present, so full screening is recommended.
How To Manage Iron Deficiency (Based on BOMSS)
1. Confirm with blood tests
- Ferritin
- Iron profile
- FBC
- B12 & folate
2. Start or adjust supplementation
Follow BOMSS dosing guidance and consider higher doses for menstruating women.
3. Review adherence
Many patients stop supplements or switch to OTC multivitamins that do not contain enough iron, zinc, or copper.
4. Consider IV iron
If:
- Oral iron is not tolerated
- Levels do not improve
- Anaemia is severe
5. Refer back to bariatric specialists if:
- Severe deficiency
- Coexisting copper/zinc abnormalities
- Persistent vomiting (risk of thiamine deficiency)
- Excessive weight loss
Dietary Tips for Patients
Although diet alone cannot correct deficiency after surgery, it helps support iron levels:
Iron‑rich foods:
- Lean red meat
- Poultry
- Fish
- Lentils, beans, chickpeas
- Spinach and leafy greens
- Iron‑fortified cereals
Enhance absorption with:
- Vitamin C–rich foods (citrus, peppers, berries)
Avoid around iron dosing:
- Tea, coffee
- Calcium supplements
- High‑calcium foods
Iron Deficiency Often Coexists With Other Deficiencies
BOMSS emphasises that iron deficiency may appear alongside:
- Vitamin B12 deficiency
- Folate deficiency
- Copper deficiency (especially if zinc intake is high)
This is why annual full nutritional screening is essential.
How Bariboost Bariatric Multivitamin Helps Reduce Iron Deficiency After Bariatric Surgery
Bariboost Bariatric Multivitamin is designed specifically to meet these needs.
BOMSS‑Compliant Iron Dose (50 mg per day)
Bariboost contains 50 mg of iron, which falls directly within the BOMSS‑recommended range of 45–60 mg daily for post‑bariatric patients. This is crucial because:
- Standard supermarket multivitamins contain only 7–14 mg of iron—far too low after surgery.
- Many patients unknowingly under‑supplement, leading to chronic deficiency.
- Menstruating women often need higher iron intake, and Bariboost’s 50 mg dose supports this increased requirement.
Why this matters: BOMSS emphasises that inadequate iron intake is a major driver of deficiency. Bariboost provides a therapeutic dose that aligns with clinical guidelines.
The UK’s most complete bariatric multivitamin
Bariboost Uses Iron Bisglycinate — And That Matters After Bariatric Surgery
One of the standout features of Bariboost Bariatric Multivitamin is its use of iron bisglycinate, a premium chelated form of iron known for superior absorption and excellent gastrointestinal tolerance. This is especially important for bariatric patients, who often struggle with both iron deficiency and the side effects of traditional iron supplements.
What Makes Iron Bisglycinate Different?
Iron bisglycinate is iron bound to two glycine molecules. This structure gives it several advantages:
✔ Higher Absorption After Bariatric Surgery
Because bariatric surgery reduces stomach acid and bypasses key absorption sites, many forms of iron (like ferrous sulfate) become harder to absorb. Iron bisglycinate, however:
- Is absorbed through different pathways than standard iron salts
- Does not require high stomach acid
- Is significantly more bioavailable in patients with altered gut anatomy
This makes it ideal for sleeve and gastric bypass patients.
✔ Gentle on the Stomach
Traditional iron supplements often cause:
- Nausea
- Constipation
- Cramping
- Metallic taste
Iron bisglycinate is known for being much gentler, with far fewer digestive side effects. Better tolerance means patients are more likely to take it consistently — and consistency is what prevents deficiency.
✔ Less Interaction With Food and Other Supplements
Iron bisglycinate is less affected by:
- Phytates
- Fibre
- Calcium
- Polyphenols (tea/coffee)
While spacing iron and calcium is still recommended, this form is more forgiving, which helps maintain stable iron levels.
✔ Clinically Proven to Improve Ferritin and Haemoglobin
Studies show iron bisglycinate:
- Raises ferritin more effectively than ferrous sulfate
- Improves haemoglobin with fewer side effects
- Is better tolerated in populations with sensitive digestion — including bariatric patients
Why This Matters for Bariatric Patients
After bariatric surgery, patients need:
- Higher iron doses
- Better absorption
- Fewer side effects
- Long‑term adherence
Bariboost’s use of iron bisglycinate directly supports all four.
Optimised Zinc–Copper Ratio to Prevent Secondary Deficiencies
Iron deficiency often coexists with zinc and copper imbalances. BOMSS recommends a zinc:copper ratio of 8–15 mg : 1 mg.
Bariboost provides:
- 20 mg zinc
- 2 mg copper
- Ratio = 10:1 (perfectly within BOMSS range)
This is important because:
- Too much zinc can cause copper deficiency
- Copper deficiency can mimic iron‑deficiency anaemia
- Balanced ratios help maintain healthy red blood cell production
Bariboost’s formulation prevents the “see‑saw effect” where correcting one deficiency triggers another.
Includes Key Cofactors Needed for Iron Utilisation
Iron doesn’t work alone. Bariboost includes several nutrients that support iron absorption and red blood cell formation:
- 800 mcg folic acid (BOMSS‑recommended 400–800 mcg)
- Vitamin B12 (critical for preventing macrocytic anaemia)
- Thiamine (protects against neurological complications)
These nutrients help ensure that iron is actually used effectively by the body.
No Calcium Included — Improving Iron Absorption
Bariboost intentionally does not include calcium, because:
- Calcium blocks iron absorption
- BOMSS instructs patients to take iron and calcium at least 2 hours apart
By separating these nutrients, Bariboost helps maximise iron uptake and reduces the risk of deficiency.
Patients can take their calcium supplement later in the day without interference.
Two Small, Easy‑to‑Swallow Capsules Per Day
Many bariatric patients struggle with:
- Large tablets
- Chewables that cause nausea
- Multivitamins with unpleasant taste
Bariboost uses vegan capsules that are:
- Small
- Nearly tasteless
- Easy to swallow
Better adherence = better iron levels.
Designed Specifically for Sleeve & Gastric Bypass Patients
The product is formulated for:
- Vertical Sleeve Gastrectomy (VSG)
- Roux‑en‑Y Gastric Bypass (RYGB)
These are the two procedures with the highest risk of iron deficiency.
Bariboost includes bariatric‑level doses of:
- Iron
- Vitamin D
- B12
- Folic acid
- Copper
- Zinc
This makes it a true “all‑in‑one” solution for long‑term micronutrient support.
Real‑World Feedback Supports Improved Energy & Symptom Relief
Customer reviews highlight:
- Increased energy
- Better tolerance than other bariatric multivitamins
- Improved adherence after years of struggling with alternatives
While anecdotal, this aligns with what we expect when iron deficiency improves.
Key Takeaways
- Iron deficiency is common, persistent, and often under‑diagnosed after bariatric surgery.
- BOMSS recommends annual blood tests for life.
- All SG/RYGB/OAGB patients require lifelong iron supplementation.
- Menstruating women need higher doses.
- Some patients will require IV iron.
- If one deficiency is found, screen for others.
- Persistent vomiting or neurological symptoms require urgent referral.
- For bariatric patients who struggle with low iron, fatigue, hair loss, or anaemia, Bariboost offers a targeted, guideline‑aligned solution.
