Heartburn and acid reflux are common concerns for people considering or recovering from weight‑loss surgery. While bariatric surgery often improves reflux symptoms, some procedures can trigger or worsen acid reflux in certain patients. Understanding the differences between gastric sleeve and Roux‑en‑Y gastric bypass can help you make informed decisions and get the right treatment if symptoms occur.
Acid reflux after gastric bypass symptoms
Roux‑en‑Y gastric bypass is often recommended for patients who already suffer from severe acid reflux. Most people experience significant improvement, but a small number may still develop symptoms months or even years later.
Symptoms of acid reflux after gastric bypass may include:
- Burning chest discomfort (heartburn)
- Sour or bitter taste in the mouth
- Food or acid coming back up (regurgitation)
- Chronic cough or hoarseness
- Trouble swallowing
If symptoms return after gastric bypass, it is important not to ignore them. Long‑term reflux can irritate the esophagus and should be evaluated by your bariatric or gastrointestinal specialist.
Roux-en-Y gastric bypass for acid reflux
Roux‑en‑Y gastric bypass is considered the most effective bariatric surgery for controlling GERD. This procedure helps reduce reflux by:
- Lowering acid production in the stomach
- Preventing bile from flowing back into the esophagus
- Reducing pressure inside the abdomen through weight loss
Many patients are able to reduce or completely stop reflux medications after surgery. For patients with obesity and frequent heartburn, gastric bypass is often the preferred option—especially when reflux symptoms are moderate to severe before surgery.
That said, continued follow‑up is important. In rare cases, anatomical changes or weight regain can cause reflux symptoms to return.
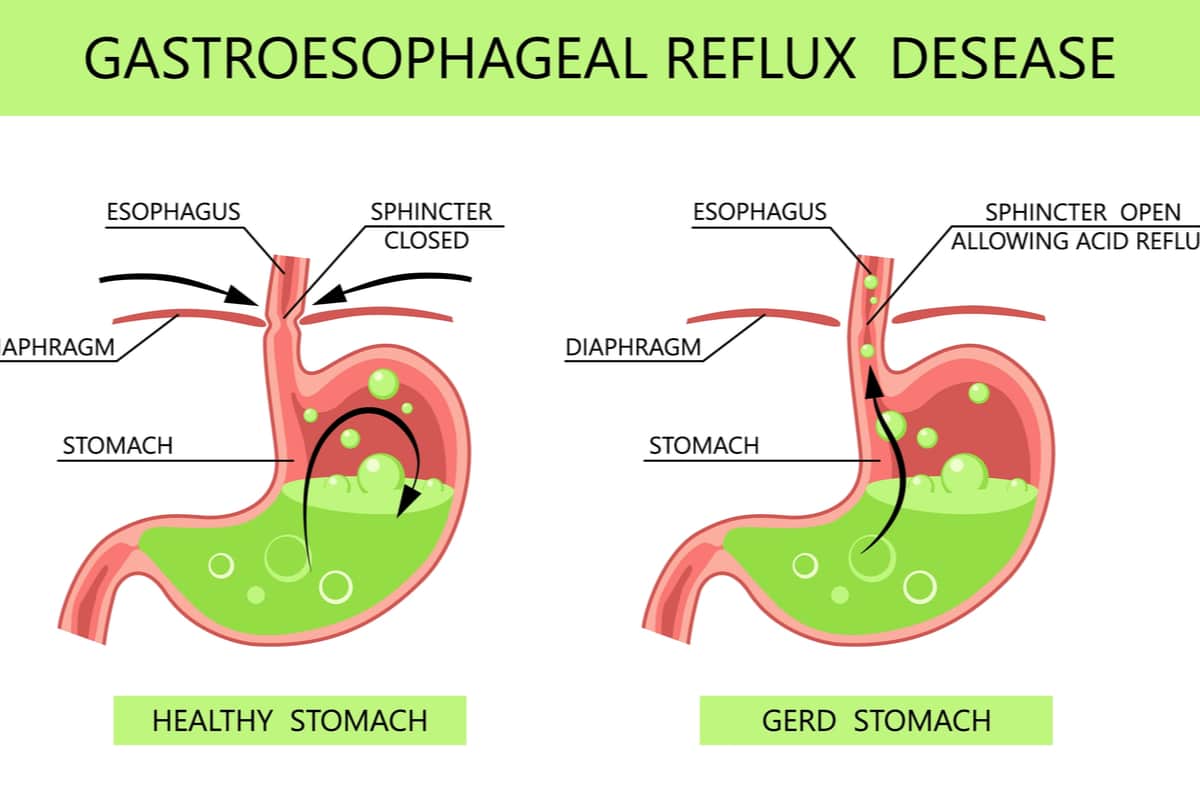
How to treat GERD after gastric sleeve
Gastric sleeve surgery is very effective for weight loss, but it may increase the risk of acid reflux in some patients. If reflux develops after sleeve surgery, treatment usually begins with conservative measures.
Treatment options include:
- Diet and lifestyle changes such as smaller meals, avoiding trigger foods, and not eating before bedtime
- Medications to reduce stomach acid, including H2 blockers or proton pump inhibitors (PPIs)
- Further evaluation with endoscopy if symptoms persist
The UK’s most complete bariatric multivitamin
For patients who continue to experience severe GERD despite treatment, conversion from gastric sleeve to Roux‑en‑Y gastric bypass may be recommended. This revision surgery is highly effective at resolving reflux while maintaining weight‑loss benefits.
Signs of acid reflux after gastric sleeve
Early recognition of reflux symptoms is key to preventing long‑term complications. Common signs of acid reflux after gastric sleeve include:
- Frequent or worsening heartburn
- Acid backing up into the throat
- Chest pain unrelated to the heart
- Night‑time coughing or choking sensations
- Nausea or vomiting after meals
If these symptoms occur regularly or worsen over time, medical evaluation is important. Your care team may recommend imaging or endoscopy to assess the esophagus and stomach.
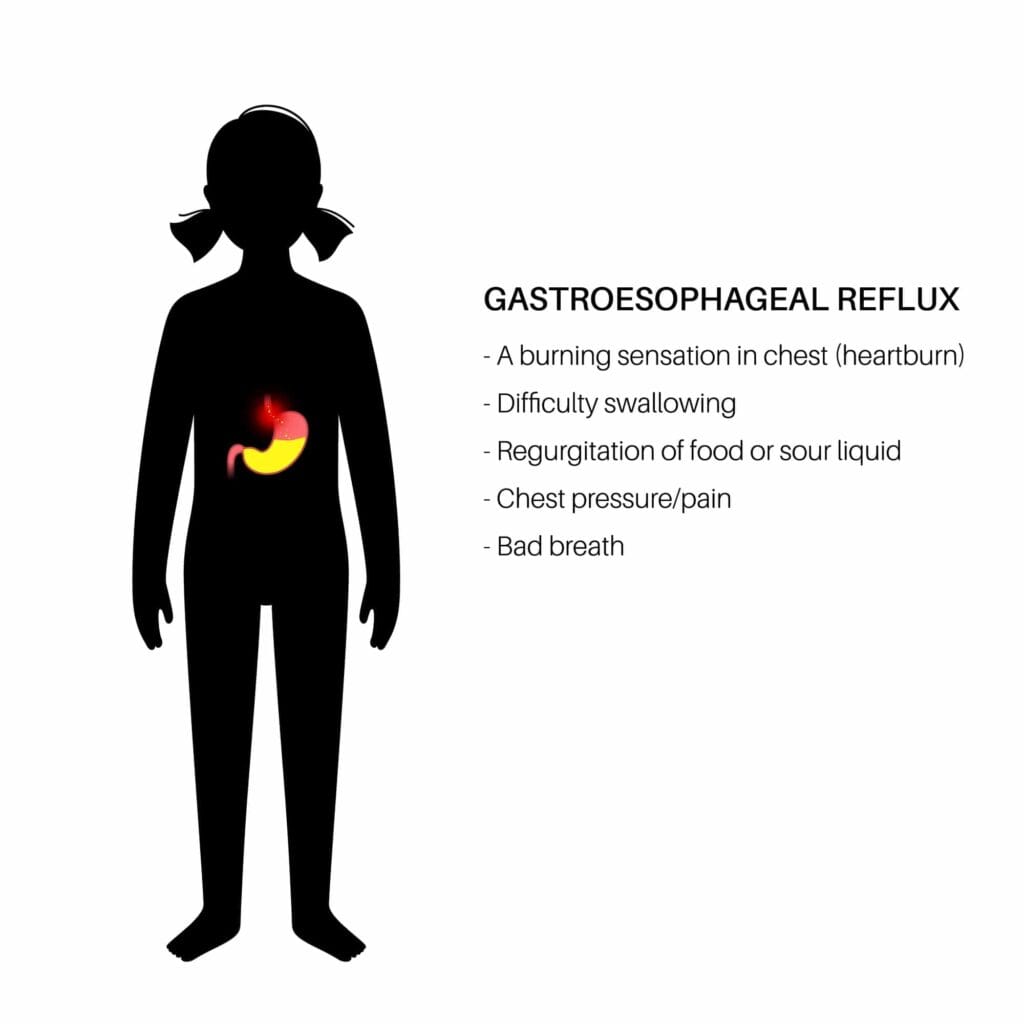
What can i take for heartburn after gastric sleeve
For many patients, heartburn after gastric sleeve can be managed safely with medication.
Common options include:
- H2 blockers such as famotidine for mild symptoms
- Proton pump inhibitors (PPIs) such as lansoprazole, omeprazole or esomeprazole for more persistent or severe reflux.
These medications are often effective, especially when combined with dietary changes. However, if you need long‑term or high‑dose medication, your provider may recommend additional testing or discuss surgical options.
When should you contact your bariatric team?
You should seek medical advice if:
- Reflux symptoms occur more than twice per week
- Heartburn does not improve with medication
- You have difficulty swallowing or persistent chest pain
- Symptoms interfere with sleep or daily activities
Early treatment leads to better outcomes and helps protect your esophagus long term.
Frequently Asked Questions About Acid Reflux After Bariatric Surgery
Yes. Gastric sleeve surgery can cause new or worsening acid reflux in some patients. The smaller, high‑pressure stomach created during sleeve surgery can make it easier for stomach acid to move upward into the esophagus. Symptoms may appear shortly after surgery or develop over time.
For patients with significant acid reflux, Roux‑en‑Y gastric bypass is usually the better option. It reduces acid exposure to the esophagus and is considered the most effective bariatric procedure for GERD relief. Gastric sleeve may worsen reflux in some people, especially those with pre‑existing heartburn.
Studies suggest that up to 30% of patients may develop new acid reflux symptoms after gastric sleeve surgery. Some patients improve with medication and lifestyle changes, while others may require further treatment or revision surgery.
For many patients, reflux improves within weeks or months as the body heals and weight loss progresses. If symptoms persist beyond a few months—or worsen—medical evaluation is recommended to prevent long‑term esophageal damage.
Concerning symptoms include:
Heartburn several times per week
Difficulty or pain when swallowing
Persistent chest pain
Night‑time reflux causing coughing or choking
Poor response to reflux medication
These symptoms should be assessed by your bariatric care team.
Proton pump inhibitors (PPIs) such as omeprazole or esomeprazole are often the most effective medications for post‑sleeve reflux. Some patients may improve with H2 blockers like famotidine. Medication choice and duration should always be guided by your healthcare provider.
Short‑term use is generally safe, but long‑term daily reflux medication should be monitored by your doctor. Ongoing symptoms may indicate an anatomical issue that requires further investigation rather than indefinite medication use.
Yes. Untreated or severe reflux can lead to esophagitis, strictures, or Barrett’s esophagus. This is why ongoing symptoms should always be evaluated rather than ignored.
Revision surgery is considered when acid reflux after gastric sleeve is:
Severe or persistent despite medication
Affecting quality of life
Causing esophageal injury
Conversion to Roux‑en‑Y gastric bypass has a high success rate in resolving reflux symptoms.
In most cases, yes. Patients with established GERD, especially those using daily reflux medication, are often advised to choose gastric bypass over gastric sleeve to reduce the risk of worsening symptoms after surgery.
Helpful steps include:
Eating smaller, slower meals
Avoiding acidic, fried, or spicy foods
Not eating late at night
Elevating the head when sleeping
Taking medications exactly as prescribed
Your bariatric team can tailor recommendations to your individual needs.
Yes. Regular follow‑up helps detect reflux early, adjust treatment, and prevent complications. Ongoing monitoring is especially important if you had reflux before surgery or develop symptoms afterward.
